Is bodybuilding too drug obsessed?
Neil Andrews says bodybuilding isn’t won with a syringe – but James Llewellin argues modern peptides are changing the game
By Gary Chappell
WHEN new Masters IFBB Pro Neil Andrews talks about drug use in bodybuilding, it carries more weight than most.
This is a man competing with a mechanical heart valve, a story already documented on Frontdouble and one that inevitably changes how he approaches enhancement, risk and longevity.
Now running what he says is just 200mg of testosterone cypionate per week, Andrews has thrown himself into one of the sport’s most sensitive debates: has bodybuilding become too drug-driven?

“This game isn’t won with a syringe”
In a recent Instagram post, Andrews did not hold back. “When did bodybuilding become so drug obsessed?" said the man who, in November last year, won his IFBB Pro Card at the European Masters in Milan.
He then listed what is fast becoming the toolkit of modern prep, before making it clear he used none of these during his last run:
- No Retatrutide
- No MOTS-C
- No HGH
- No L-carnitine
- No SLU-PP-2
And he said: “Bodybuilding has become heavily drug-driven, no denying that. But let’s get one thing straight. Nothing replaces hard work, consistency and going to those dark places others avoid. No drug, no peptide, no protocol is going to do that for you.
"It won’t build grit. It won’t build discipline. And it won’t carry you through prep when you’re exhausted, flat and questioning everything.
"You know why I stand on that? Because last year I beat guys across multiple shows, federations and internationally running 10 times what I was."
Andrews then delivered his most pertinent point: “This game isn’t won with a syringe.
"It’s won with mindset, execution and who’s willing to suffer longer. Get comfortable being uncomfortable."
For Andrews, the argument is rooted in experience, not theory. And it is a message that cuts directly against the current direction of the sport, where newer compounds and peptides are becoming increasingly mainstream.
Even in commercial gyms across the country, bodybuilders will be asked about performance-enhancing drugs long before diet and training are even at a basic, structured level.

Enter an Olympia voice and the 'peptide rabbit hole'
But the response from former 212 Mr Olympia competitor James Llewellin (above), who is set to return to the stage in the amateur ranks at May's PCA Universe this season, shows just how much the landscape has shifted.
While Llewellin did not disagree with the fundamentals of Andrews' argument, he went on to post a compelling narrative in support of peptides.
Responding directly to Andrews, Llewellin said: "Firstly, incredible conditioning mate and, secondly, until a few months ago I would have said exactly the same.
"In fact I still do. Nothing beats hard work, no drug, no peptide nothing. But when you start to go down the whole peptide rabbit hole, it’s quite remarkable what these signaling peptides can do. And not just performance enhancing.
"Nothing beats gear for muscle gains. Nothing. There isn’t a peptide out there that can really build muscle."
Health vs performance
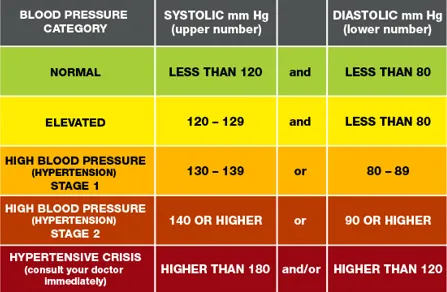
Llewellin continues: "But there are some incredible peptides that are able to up-regulate metabolism, increase mitochondria function, reverse fatty liver, improve cholesterol, regulate blood sugar, lower blood pressure and decrease body fat.
"Peptides are of huge benefit for not only health but also longevity. The exact opposite of what AAS do to you.
"At 53 years old and with two kids, my health has never been so important to me and using less anabolics and conventional fat burners was always the goal for this “comeback” prep.
"Peptides aren’t hormones, they are amino acids that signal the body to do things better and more efficiently. I’ve been super impressed with them. I’ve never felt so good on prep at this [level of] body fat.
"I feel like I’m [in my] off-season, yet normally I’d be killing myself with 1-1.5 hours of cardio a day with my inflammation through the roof. I’d be moody, quiet and not really present for my family. That’s never a good thing.
"Delve a little into them, Neil, even if it’s just for your health. It can always be tweaked and improved no matter how healthy you are.
"Yes hard work and consistency will never be beaten but, when you combine that with less gear and certain peptides, the results can be pretty amazing."
Two philosophies. One sport
What makes this exchange compelling is that both sides agree on the fundamentals: hard work wins, discipline matters and there is no shortcut
But they diverge on one crucial question: Are modern compounds enhancing the process, or replacing it?
Andrews’ position is shaped by something most competitors never face. Competing with a mechanical heart valve forces a level of restraint and realism that cuts through bodybuilding’s usual bravado.
Llewellin's argument, however, reflects where the sport is heading; less reliance on high-dose anabolic stacks, more interest in metabolic and signalling compounds, greater focus on health markers. Not instead of hard work but alongside it.
This is not a case of right vs wrong, it is a shift. Competitive bodybuilding is no longer just food, training and steroids. It is becoming hormones, peptides, metabolism and health optimisation
And the question now is not whether drugs are part of the sport. It’s how much is too much and what actually matters most?






Leave a Reply